Women experience unique hormonal fluctuations throughout life, and those shifts play a powerful role in sleep quality, breathing during sleep, and daytime energy. Yet many women’s sleep concerns are dismissed as “stress,” “aging,” or “just hormones.”
In reality, hormonal changes can influence airway stability, body temperature regulation, mood, and sleep architecture. This makes women more vulnerable to poor sleep and, in some cases, obstructive sleep apnea (OSA). A 2024 survey found that 50% of women aged 45–64 report sleep disruption related to menopause.
Understanding the hormone–sleep connection is key to early identification, effective treatment, and better well‑being.
How Do Hormones Affect Sleep?
Hormones act as the body’s chemical messengers. When estrogen, progesterone, melatonin, and cortisol shift, so does the body’s sleep-wake rhythm and nighttime breathing patterns.
Key hormones involved in sleep
- Estrogen: Helps regulate temperature and REM sleep; influences airway muscles.
- Progesterone: A natural respiratory stimulant that supports stable breathing during sleep.
- Melatonin: Controls the sleep-wake cycle.
- Cortisol: Impacts alertness, stress response, and sleep onset.
When these hormones fluctuate, sleep often fluctuates too.
Hormonal Stages That Impact Women’s Sleep
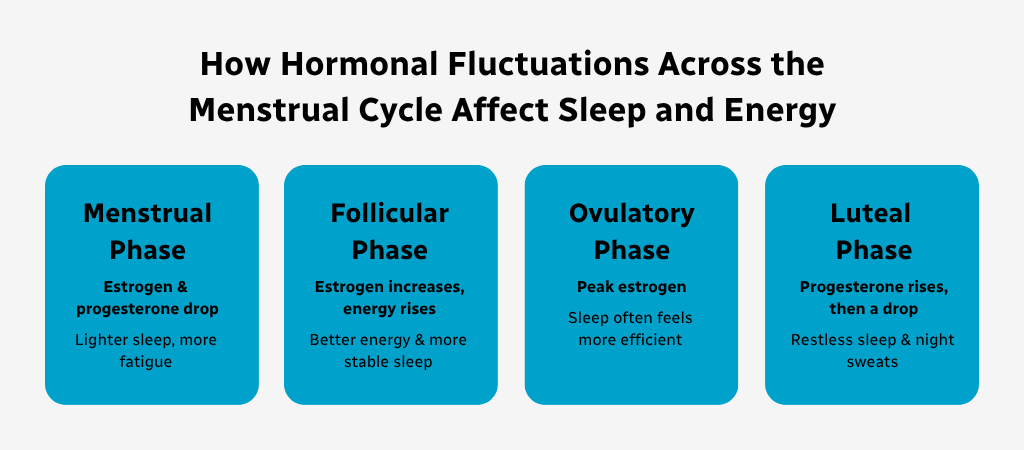
1. Menstrual Cycle
Hormonal dips in estrogen and progesterone during the late luteal phase can lead to lighter, more fragmented sleep, night sweats, increased breathing instability, and greater fatigue the following day, and women with premenstrual symptoms may notice these sleep issues more intensely.
2. Pregnancy
Pregnancy causes major increases in estrogen and progesterone, yet sleep often becomes more challenging, with common disruptors such as nasal congestion linked to higher estrogen, an increased risk of snoring, more frequent nighttime awakenings, and a higher chance of developing gestational obstructive sleep apnea, and for some women, pregnancy is the first time symptoms of sleep‑disordered breathing appear.
These early symptoms and sleep challenges are described in more detail in our guide on pregnancy, postpartum, and early motherhood, which highlights how fatigue, nighttime awakenings, and breathing changes affect women during this stage.
3. Perimenopause
Perimenopause can begin earlier than many expect, sometimes as early as the early 30s, and may last several years (typically 3 – 5 years before menopause occurs). During this transition, estrogen and progesterone fluctuate widely, and these swings can significantly disrupt sleep. Common symptoms include hot flashes, night sweats, difficulty staying asleep, mood changes, and new snoring or breathing disturbances. For some women, these hormonal shifts also make nighttime breathing less stable; increased airway collapsibility during perimenopause can raise the risk of developing obstructive sleep apnea, especially when fatigue, morning headaches, or unrefreshing sleep start to appear more consistently.
4. Menopause
During menopause, estrogen and progesterone levels decline quickly, leading to noticeable changes in sleep and nighttime breathing. Many women experience hot flashes, night sweats, more frequent awakenings, and new or increased snoring. These hormonal shifts can make breathing during sleep less stable, which may contribute to the onset or worsening of obstructive sleep apnea.
As described in our menopause‑focused sleep apnea overview, these changes can develop gradually and are often mistaken for typical aging, which makes early awareness and evaluation especially important.
5. Postmenopause
After menopause, estrogen and progesterone remain consistently low, and these long‑term hormonal changes can increase airway collapsibility and raise the risk of obstructive sleep apnea. Women may notice ongoing snoring, lighter sleep, frequent awakenings, or reduced sleep efficiency. Because symptoms develop gradually and often resemble typical aging, they are easy to overlook without a proper sleep assessment.
Why Hormonal Changes Increase the Risk of OSA
While OSA is often viewed as a “men’s health” issue, hormone‑driven changes in airway structure and muscle responsiveness mean women are uniquely affected, especially during perimenopause and menopause.
How hormone changes influence OSA risk
- Lower estrogen reduces airway muscle tone
- Reduced progesterone decreases respiratory drive
- Weight redistribution around the neck after menopause can narrow the airway
- Hot flashes disrupt sleep and mask underlying OSA symptoms
Women’s OSA symptoms often differ from men’s, making it harder to identify. Instead of loud snoring, many women report:
- Insomnia-like symptoms
- Morning headaches
- Fatigue or low energy
- Difficulty concentrating
- Nighttime awakenings
How to Improve Sleep During Hormonal Changes
1. Support your sleep environment: Keep your bedroom cool, use breathable bedding, and reduce light exposure in the evening to support a more comfortable and restful sleep environment.
2. Strengthen your sleep routine: Aim for a consistent wake time each day, as this helps anchor your body clock. Rather than going to bed at a fixed time, wait until you feel genuinely sleepy before turning in. Limit caffeine later in the day and prioritize wind‑down activities that reduce stress and help your body transition naturally into sleep.
3. Monitor symptoms of disrupted breathing: Look for signs such as snoring, waking up unrefreshed, morning headaches, daytime sleepiness, or waking up gasping or choking, as these symptoms may indicate an underlying sleep‑related breathing issue.
Read more on our blog Signs You May Have a Sleep Disorder.
4. Consider a home sleep test if symptoms persist: Home sleep testing can help identify obstructive sleep apnea, especially during midlife transitions when symptoms often appear or worsen.
If sleep issues are impacting your quality of life, a Resolve sleep clinician can help determine whether a home sleep test is appropriate.
5. See your Primary Care Practioner or Gynecologist if symptoms persist: Modern approaches to safe pharmacotherapy including plant-based hormones are available and are not only extremely effective but do not carry the risk of endometrial cancer that older higher levels of estrogen therapy used to.
Frequently Asked Questions
Hormones influence temperature regulation, breathing stability, melatonin production, and mood. When estrogen and progesterone fluctuate, women may experience lighter sleep, frequent awakenings, or symptoms that resemble insomnia or obstructive sleep apnea (OSA).
Rapid swings in estrogen and progesterone can trigger night sweats, mood changes, and airway instability. These shifts make sleep more disrupted and may increase the risk of snoring, chronic insomnia, or obstructive sleep apnea.
Hormonal changes don’t directly cause OSA, but declining estrogen and progesterone can make the airway more collapsible during sleep. Weight gain in midlife, especially around the neck and upper airway, can further narrow the airway and increase chronic insomnia or OSA risk.
A cool sleep environment, consistent sleep habits, and monitoring for breathing symptoms can help. If snoring, fatigue, or disrupted sleep persist, a sleep test may help determine whether OSA is contributing.

